
At FLYRCM, we are redefining the future of healthcare revenue cycle with machine learning, large language models, and autonomous agents. Please watch our video demo to learn more about how we are accomplishing this goal.
FLYRCM Demo Video
FlyRCM revolutionizes the healthcare revenue cycle, smoothing out traditional points of friction encountered by clinicians and healthcare professionals. By harnessing advanced automation and intelligence, FlyRCM enhances the financial vitality of health systems. This innovative approach not only uplifts healthcare professionals but also elevates the overall patient care experience.
Our Mission:
To harness the transformative potential of AI in optimizing the healthcare revenue cycle, paving the way for a more efficient and proactive financial landscape in the healthcare sector. In short, we want to fix this graph below from KFF.
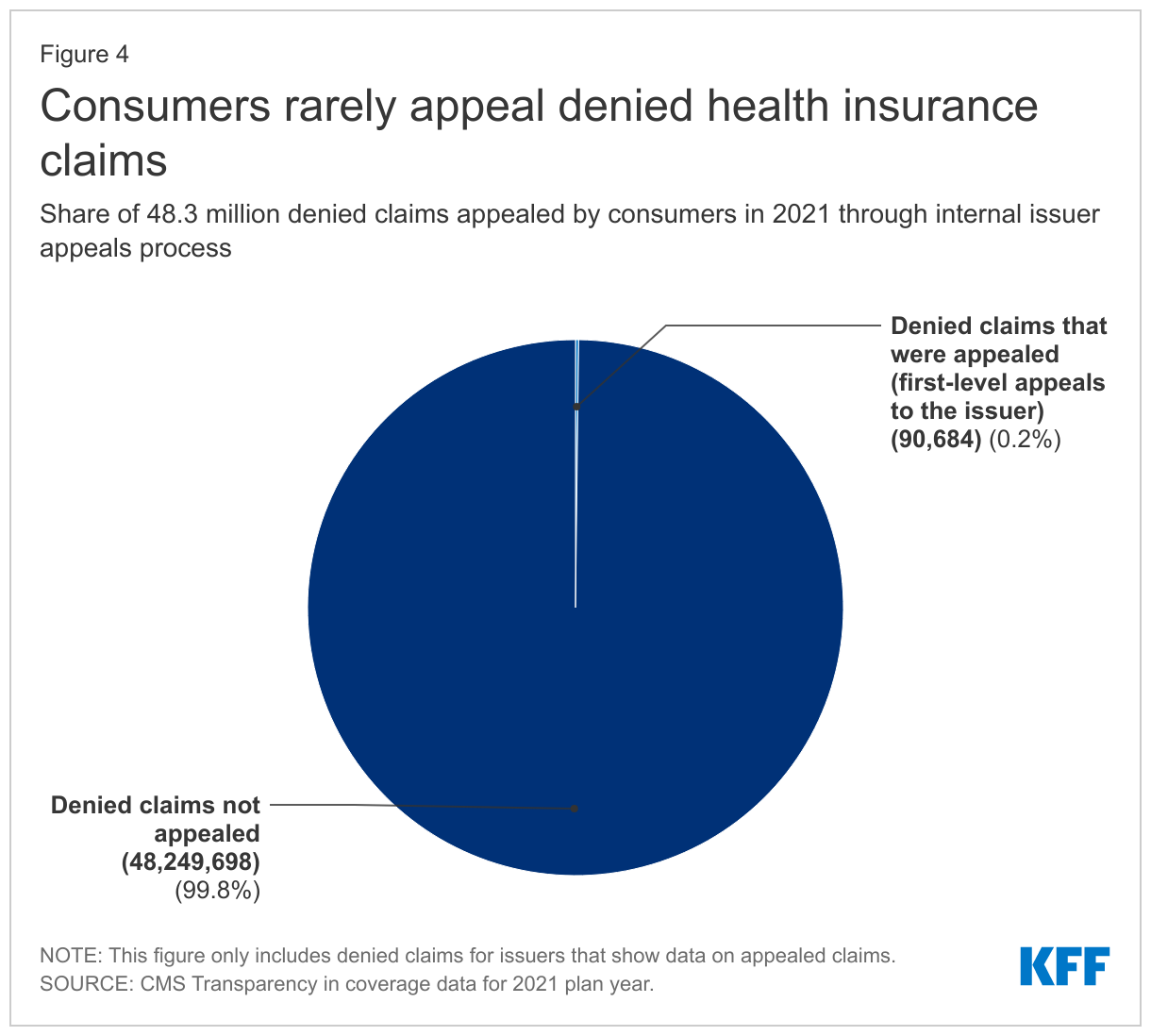
Our Milestones:
- Multiple Automated Workflows: A testament to our drive for innovation and efficiency.
- 1000+ Analyzed Claims: Every claim we analyze further enriches our database, sharpening our predictive analytics, and providing an improved strategy for future claims.
- 100% Professional & Dedicated: Our team embodies professionalism and passion, ensuring our clients receive unparalleled service.
Our Services:
- Automated Denial Tracking: Our AI-driven system identifies and logs denied claims, neatly categorizing them for streamlined reference and action.
- Standardized Appeals: We offer ready-to-use, prefilled templates for various appeal scenarios. This not only accelerates the appeal process but ensures the documentation is error-free.
- Appeal Monitoring: We prioritize transparency. Our system allows healthcare providers to check the status of their appeals instantly.
Why Choose Us:
Addressing denied claims in healthcare has long been a significant challenge. With our AI-driven tools, this traditionally time-intensive process has been reduced to mere moments. This isn't just about speed; it's about preemptively identifying potential challenges to ensure smoother operations. The result is a swift appeals process, minimized errors, and maximized revenue recovery. We're not just setting a new standard in healthcare finance; we're setting the gold standard.
FAQs:
- How does AI enhance the healthcare claims process?
AI accelerates the claims process by swiftly recognizing and organizing denied claims. Additionally, it pre-fills paperwork, helping in faster resolutions and preemptive error detection. - Does AI replace human intervention in the appeals process?
While AI significantly streamlines the process, human expertise remains essential for decision-making and oversight. AI acts as an assistive tool, not a total replacement. - How secure is our data with FLYRCM's AI-driven tools?
We place paramount importance on security. Our AI tools incorporate advanced encryption and adhere to stringent data privacy regulations, ensuring all patient and financial information remains protected. - How does winning more claims boost our platform's efficiency?
Every victorious case augments our platform's database. As we amass more data, our predictive analytics becomes more acute, letting us predict potential claim challenges and suggest effective solutions.
Join us on our journey as we revolutionize the healthcare revenue cycle, making it more efficient, transparent, and profitable. FLYRCM - The future of healthcare finance is here.

